PROTECT YOUR DNA WITH QUANTUM TECHNOLOGY
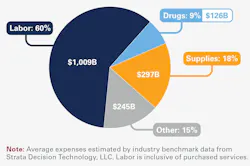
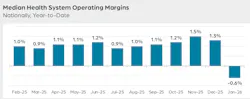
Orgo-Life the new way to the future Advertising by AdpathwayU.S. hospital and health system finances are entering 2026 in a fragile position, burdened by administrative complexity, cost pressures, widening provider disparities, more and sicker patients, and rising labor costs. Is this just a phase, or will it persist? April 27, 2026 18 min read ID 18291399 © Sean Pavone | Dreamstime.com • Hospital and health systems face persistent operating margin pressure and widening disparities across providers. While revenues have improved, underlying challenges continue to constrain profitability. • Where care is delivered has been changing, with more services moving to lower-acuity settings outside the hospital — and outpatient revenue growth continues to exceed inpatient revenue increases. • Labor costs have increased because base salaries and wage expenses continue to rise for staff retention. • The payer mix has shifted as an increase in uninsured patients and a movement toward government payers, such as Medicare and Medicaid, versus private insurance has lowered net operating revenue. • Hospitals are dealing with the administrative burdens, rising uncompensated care and increased costs associated with insurance claim denials. Hospitals and health systems are the backbone of U.S. healthcare. While their finances have stabilized since COVID-19, they’re still fragile. The industry has entered a period defined by razor-thin margins, ongoing cost pressures, widening provider disparities and increased administrative burdens. During 2024 and 2025, patient volumes returned, elective procedures rebounded and revenue growth resumed. But beneath that improvement is a more complicated reality: operating margins — a measure of how well an organization manages revenue relative to operating expenses — are at historically low levels, often hovering around 1%. Let’s take a closer look at what’s happening and why. Hospital and health system operating margins are stabilizing in 2025-2026, settling into a “new normal” defined by higher patient volumes and mounting expense pressures, according to Kaufman Hall’s “National Hospital Flash Report: February 2026.” Margins remain narrow due to high labor, drug and supply costs, with many smaller or rural hospitals continuing to struggle. Some of the report’s key findings include: • Cost pressures are creating a shaky financial outlook. Hospital expenses are elevated in early 2026 compared to 2025, while revenues are pressured by an eroding payer mix and remain below sustainable levels. • Softer, uneven volumes reflect shifting care patterns. Patient days have softened in early 2026, while the average length of stay remains steady, reflecting both demographic shifts and changes in where care is delivered. • Outpatient revenue is rising in early 2026. Outpatient care offers significant benefits to both patients and health systems, though hospitals must manage lower reimbursement per case and a greater concentration of high-acuity patients. In addition, the latest annual American Hospital Association’s (AHA) Costs of Caring report confirms hospitals and health systems continue to face increases in the costs of labor, supplies, medicine and infrastructure needed to adequately provide care and services. Highlights from the report include: Source: American Hospital Association Workforce spending remained hospitals’ top expense in 2025. Source: American Hospital Association. • Labor spending remains the top expense. About 60% of total expenses went to paying doctors, nurses, specialists and other professionals. In 2025, labor costs rose 5.6% from the previous year. • Hospital costs to care for patients grew twice as fast as hospital prices. In 2025, hospital expenses grew 7.5%, more than twice the rate of growth in hospital prices. Hospital expenses for supplies increased 9.9% and drugs increased 13.6%. • Hospitals are caring for more patients who are sicker. From 2019 to 2024, about 36% of hospital expense growth came from higher patient volumes, and 19% of the increase came from treating sicker, more complex patients requiring increased staff time, monitoring and specialized care. • Hospitals spend billions to address administrative burden from insurer claims denials and prior authorization. Hospitals in 2025 spent $43 billion trying to collect payments from insurers for care already delivered. Excessive prior authorization requirements, claims denials and payment delays; repeated documentation requests; and evolving billing and coverage rules have contributed to these mounting expenses. • Most hospital costs are tied to service lines where reimbursement falls short of the cost of delivering care. About 56% of hospital costs are tied to service lines where reimbursement is less than the cost of delivering care, including behavioral health, obstetrics, infectious disease, and burns and wounds. Against this backdrop, a clear divide is emerging. Large, well-capitalized health systems with scale, strong payer contracts and advanced operational capabilities are maintaining healthy margins. Meanwhile, smaller, rural and safety-net hospitals are struggling to stay afloat. This widening gap is one of the most important trends in the sector. It suggests financial performance is becoming less about cyclical recovery and more about structural positioning. Scale, efficiency and payer leverage are increasingly determining which organizations can thrive and which are at risk. According to research from the recent “Performance Trends Report” from Strata Decision Technology, covering Q4 2025 through January 2026, health system operating margins declined sharply to begin 2026, due in part to month-over-month revenue decreases that outpaced expense declines. Key takeaways for the four months covered in this report include: • Health system operating margins held below breakeven levels at -0.3%, up only slightly from -0.6% in January. • Supply and drug expenses were key drivers of ongoing expense growth, rising 7.8% and 7.6% Y-o-Y and contributing to a 5.7% increase in total expense. • Revenue growth reflected continued strength in outpatient care, with gross operating revenue increasing 6.0% Y-o-Y, including a 7.2% rise in outpatient revenue. • Physician practices felt the weight of sustained financial strain, as rising expenses and limited physician productivity gains pushed needed investment levels higher. The median year-to-date operating margin of -0.6% in January 2026 is down from 1.3% in December 2025. This marks the largest month-over-month decline in more than 12 months and represents a notable shift from 2025, when operating margins remained within a few tenths of a percentage point of 1% for most of the year. Source: Strata Comparative Analytics The median year-to-date operating margin fell to -0.6% in January 2026, down from 1.3% in December 2025. This marks the largest month-over-month decline in more than 12 months. Source: Strata Comparative Analytics Operating margins also weakened at the individual hospital level in January. The median change in hospital operating margin declined 2.4 percentage points Y-o-Y and 3.1 percentage points month over month. While smaller hospitals typically experience the most pressure and lower margins, performance varies widely. Some large systems outperform significantly, but even among them, results are inconsistent, as you’ll see in the list below. And the systems showing operating margins above 5% are outliers, as most health systems are balancing razor-thin margins. Here are examples of hospital and health system margins that give a glimpse into the disparity between larger systems and smaller or mid-size systems. Tenet Healthcare. This health system recorded a 2025 operating income of $3.5 billion, with a 16.5% operating margin. This is lower than its 2024 margin at 28.8%, based on $6 billion in operating income and driven by strong ambulatory care growth, high-acuity procedures and the divestiture of 14 hospitals. Its 2023 margin was lower at 12.2%. Tenet Health is one of the largest U.S. health systems, operating more than 50 hospitals and 535 ambulatory surgery centers/surgical hospitals, with about 86,000-100,000 employees and revenues exceeding $20 billion. HCA Healthcare. HCA’s full-year operating margin reached 13% according to industry reports, while other financial trackers listed it around 15.9% for the fiscal year ending Dec. 31, 2025. This reflects revenue of $75.6 billion. For 2024, HCA reported an operating margin of 12.1%, up from 11.9% in 2023. HCA Healthcare is the largest for-profit U.S. health system, operating 190 hospitals and about 2,400 ambulatory sites (surgery centers, urgent care, clinics) in 20 states and the UK. Based in Nashville, it employs more than 309,000 people and manages ~44 million annual patient encounters. Mayo Clinic. For the three months ending Sept. 30, 2025, the medical center posted an operating margin of 8% and operating income of $442 million. The system reported a record-setting 6.5% operating margin for 2024, with $1.3 billion in operating income on $19.8 billion in total revenue. This represents an increase from 2023's 6% margin, driven by high patient demand and a $10.5 billion investment in labor. Mayo Clinic is a nonprofit academic medical center known for integrated clinical care, research, and medical education. Based in Rochester, Minnesota, it operates major campuses across several states and is recognized for its patient-centered, team-based approach, where specialists collaborate to diagnose and treat complex conditions. NewYork-Presbyterian/Weill Cornell Medical Center. This health system recorded a 3.9% operating margin in Q3 2025, driven by $2.9 billion in revenue and $115 million in operating income, affected by rising costs. It’s lower than its 4.5% operating margin in Q3 2024, which was higher than the 3.3% in the same period of 2023. NewYork-Presbyterian/Weill Cornell is a major academic medical institution in Manhattan, featuring 862 beds. It is a top research and teaching hospital, acting as a key component of the NewYork-Presbyterian healthcare system that operates more than 4,000 beds across its various locations. University of Pittsburgh Medical Center (UPMC). UPMC recorded an operating margin of 0.9% for the full year 2025, rebounding from a 2024 margin of -1.1% and 2023 margin of about -0.7%. UPMC is a massive nonprofit health system and insurer based in Pittsburgh, with 100,000 employees, more than 40 hospitals, more than 800 outpatient sites and a large insurance division serving four million members. Kaiser Permanente. For the three months ended Sept. 30, 2025, Kaiser Permanente’s operating margin was 0.7%, with operating income of $218 million. This is an increase from its operating margin loss of -2.1%, or $608 million margin during the same period in 2024. Kaiser Permanente is one of the largest nonprofit healthcare systems in the United States, combining health insurance plans with hospitals and physician groups under a single integrated model. It focuses on coordinated, preventive care, serving millions of members across multiple states. Allegheny Health Network. Pittsburgh-based Allegheny Health Network recorded a 0.5% operating margin on an operating income of $7 million in Q3 2025, up from a margin loss of -2.4% and operating loss of $30.9 million during the same period 2024. Allegheny Health Network is a mid-to-large regional health system and one of the largest healthcare providers in the Pennsylvania region. It’s a nonprofit, integrated healthcare system that operates a network of hospitals, outpatient centers and physician practices, with 14 hospitals, about 2,600 physicians and 23,000 employees. Providence. Renton, Washington-based Providence reported an operating margin of 0.3% with operating income of $21 million in Q3 2025, up from an operating margin loss -2.7%, or $208 million, during the same period in 2024, according to its Nov. 13 financial report. It’s a large nonprofit health system that operates a broad network of hospitals, clinics and physician groups across the western United States, with more than 50 hospitals, about 120,000 physicians and clinicians, and more than 1,000 sites of care. UnityPoint Healthcare. For Q3 2025, West Des Moines, Iowa-based UnityPoint Health reported an operating loss of $17 million and a -1.3% operating margin, reflecting ongoing expense pressures that outpaced revenue growth. For the nine months ending Sept. 30, 2025, the system recorded a -0.5% margin loss and $20.8 million operating loss, down from a 2.2% margin and $84.9 million gain Y-o-Y. UnityPoint Health is a nonprofit, integrated healthcare system that provides coordinated care across hospitals, clinics, and home-based services throughout the Midwest. It has about 18 hospitals, 3,000 physicians and practitioners, 30,000 employees and more than 400+ sites of care, including clinics, outpatient centers and home care services. Centene Corp. Not all margin pressures are confined to providers. For example, this health system reported a -3.9% operating margin for full-year 2025, driven mostly by impairment charges and rising medical costs. The 2025 margin is down from its 2024 margin of 1.96%. Centene Corp. is a U.S., for-profit managed-care organization and Fortune 500 company specializing in government-sponsored healthcare programs. It’s a major intermediary for Medicaid, Medicare and Health Insurance Marketplace plans, serving more than 27 million members in all 50 states. With these margins in mind, labor accounts for the largest share of hospital expenses and continues to weigh heavily on financial performance. Hospitals are now operating with a permanently higher labor cost base. The Strata Decision Technology report indicates health systems increased compensation and benefits to attract and retain staff even as productivity levels remain steady. At the same time, non-labor expenses — from pharmaceuticals to medical supplies — continue to accelerate. Specialty drugs, in particular, have become a major cost driver, often outpacing reimbursement. The result is a persistent imbalance: expenses are growing faster than revenue, squeezing margins. Source: Strata Comparative Analytics Non-labor expenses, shown here from Q1 2024 through Q4 2025, continue to rise, and specialty drugs have become a major cost driver, often outpacing reimbursement. Source: Strata Comparative Analytics A big challenge is that the payer mix has shifted in ways that are difficult for hospitals to control. A larger share of patients is covered by Medicare and Medicaid, which typically reimburse below the cost of care. Meanwhile, hospitals are seeing increases in uncompensated care and bad debt, reflecting broader economic pressures on patients, according to the Strata Decision Technology report. Even when volumes are strong, the revenue generated per patient is often lower than in the past. As mentioned earlier, where care is delivered has been shifting, with more services moving to lower-acuity settings outside the hospital. The AHA report showed that outpatient visits in 2025 rose 9.8% Y-o-Y. The Strata Decision Technology study reveals that outpatient revenue growth continued to exceed inpatient revenue increases, reflecting the evolving shift. While the change can improve efficiency and reduce costs, it’s also putting pressure on hospital margins. Outpatient care typically generates lower reimbursement, while inpatient facilities are increasingly reserved for the most complex and costly cases, leaving hospitals to manage a sicker patient population with a less favorable financial profile. “Medicare changed some reimbursement qualifications,” says Steve Wasson, chief data and intelligence officer at Strata Decision Technology. “Services and procedures that used to only be reimbursed in the inpatient setting can now be reimbursed in the outpatient setting,” Another factor supporting the increasing use of outpatient services is that costs for outpatient care often are lower, so operating margins are typically higher than hospitals and health systems.” — Steve Wasson, Chief Data and Intelligence Officer, Strata Decision Technology Wasson says technological advances and new approaches to care delivery make it possible to perform many procedures in outpatient settings. “Providers can deliver the same level of care without extended hospitalization, and patients prefer the convenience of coming in for a day or a short overnight stay, depending on their needs, and returning home sooner,” he notes. As a result, some hospitals and health systems are investing in buying or building outpatient organizations and facilities to stay competitive. Wasson recommends buyers consider capital investments carefully. “Consider how you're going to deploy your capital expenditures into those spaces,” he says, “whether you want to buy or build a surgery center, or if you want to partner with an outpatient setting, carefully analyze investments if you want to be competitive in the next several years.” The story of hospital margins now is about recalibration. The industry is struggling with deep, persistent challenges. How health systems respond, including through cost discipline, strategic focus and operational innovation, will determine whether this period of thin margins becomes a temporary phase or a long-term reality. Looking ahead, most analysts expect continued margin stability with ongoing pressure, and include these observations and point to several key trends: • Margins are unlikely to return to pre-pandemic levels in the near term. • Policy changes, especially Medicare and Medicaid funding, could create downside risk. • Financial performance will increasingly depend on: o Cost discipline and labor optimization. o Revenue cycle improvements. o Service line mix and ambulatory strategy. o Scale and partnerships. As a result, hospitals must simultaneously manage rising costs, shifting care models and unfavorable reimbursement dynamics — all while continuing to invest in digital, outpatient, and value-based care capabilities that will define long-term competitiveness. Theresa Houck, Senior Editor, is an award-winning B2B journalist with more than 35 years of experience. She writes about strategy, policy, and economic trends for EndeavorB2B on topics including healthcare, cybersecurity, IT, OT, AI, manufacturing, industrial automation, energy, and more. With a master’s degree in communications from the University of Illinois Springfield, she previously served as Executive Editor for four magazines about sheet metal forming and fabricating at the Fabricators & Manufacturers Association, where she also oversaw circulation, marketing, and book publishing. Most recently, she was Executive Editor for the award-winning The Journal From Rockwell Automation publication on industrial automation where she also hosted and produced podcasts, videos and webinars; produced eHandbooks and newsletters; executed social media strategy; and more 
Key Highlights
Key Operating Margin Trends, 2025-2026
Deep Dive: Margins Take a Downturn to Start 2026
Profit Margins from Real Hospitals, Health Systems
Labor is the Industry’s Weighty Anvil

Outpatient Care Continues to Grow

Outlook: Stable but Fragile
About the Author

Theresa Houck
Senior Editor

.jpg)











 English (US) ·
English (US) ·